Start Improving Your Health in Minutes.
Start Improving Your Health in Minutes.
Library
FEATURED
HEALTH HIGHLIGHT
FEATURED

Understand your triggers, find relief that works, and stop migraines from ruling your life.
HEALTH HIGHLIGHT

Learn how to protect your bones, reduce risk of fractures, and take charge of your bone health at any age.
MINI GUIDES

Get quick answers, learn proven tips, and take action with our bite-size mini guides.
Understanding Migraine Headache Symptoms: A Clear Guide
February 15, 2026 13 min read

Searching online for information about migraine headache symptoms can be a frustrating experience. You are often met with long, disconnected lists of symptoms or conflicting advice that leaves you feeling more confused than when you started.
A migraine is not just a severe headache. It is a complex neurological event with distinct phases, and the head pain is often just one part of a much larger process. Symptoms can begin hours or even days before the headache and linger long after the pain has subsided.
This guide aims to provide clarity. We will explore migraine symptoms through the lens that healthcare professionals use—not as a random collection of issues, but as a structured sequence of events. Understanding this pattern can help you make sense of your own experiences.
The goal here is not to offer a diagnosis, but to give you a reliable framework. A powerful first step in managing migraines is to track your symptoms and identify personal patterns. Using a structured migraine diary template is an effective way to begin this process.
By focusing on the 'why' behind the symptoms, you can start to feel more in control. This understanding empowers you to have clearer, more productive conversations with your doctor about what you are experiencing.
Let's walk through the key signs of a migraine attack and the underlying brain processes, providing a grounded perspective on what can feel like a chaotic and overwhelming condition.
What Is a Migraine? A Neurological Event
It is common to think of a migraine as just a very bad headache, but that doesn't capture the full picture. In clinical settings, a migraine is understood as a complex neurological event that originates in the brain but can affect the entire body. The intense head pain is perhaps the best-known symptom, but it is only one component.
Think of it less like a typical tension headache and more like a temporary, spreading wave of altered nerve activity in your brain. This event can affect blood vessels and activate major pain pathways.
This chain reaction is what produces the wide-ranging symptoms associated with a migraine, from visual disturbances and sensory sensitivity to nausea and cognitive fogginess.
More Than Just Pain
Recognising that a migraine is fundamentally neurological helps explain why it feels so different from other headaches. It clarifies why symptoms can appear long before any pain starts and persist after the headache has faded. The underlying mechanisms are a significant area of research, and learning what causes frequent migraines can offer further insight into these processes.
You are not alone in this experience. Migraine is one of the most common neurological conditions in the UK, affecting an estimated 10 million people aged 15 to 69. To put this in perspective, it is more widespread than diabetes, asthma, and epilepsy combined. This results in around 2.5 million GP appointments annually, highlighting its impact on individuals and the healthcare system. The NHS continually refines its approach to improved migraine care.
A migraine attack is not just a symptom; it is an experience. The pain, nausea, and sensitivity are all outward signs of a complex event unfolding within the brain’s intricate networks.
The Brain's Electrical Cascade
This neurological event is sometimes compared to a type of electrical storm. It often begins with a wave of heightened nerve cell activity spreading across the brain's surface, followed by a period of suppressed activity. This process is known as cortical spreading depression.
As this wave travels, it can temporarily disrupt the function of the brain region it passes through. This mechanism helps explain the variety of symptoms people report. For example:
- If the wave crosses the visual cortex at the back of the brain, it may trigger the visual disturbances known as an aura.
- If it moves through the brainstem, it might be responsible for symptoms like dizziness or nausea.
- When it activates the trigeminal nerve—a primary pain pathway for the head—it sets off the severe, throbbing pain that is the hallmark of a migraine.
Viewing a migraine this way helps shift the focus from simply treating the pain to understanding and managing the entire sequence of events.
The Four Phases of a Migraine Attack
A migraine is not a single event but a process that unfolds in stages, often over several hours or even days. Learning to recognise this sequence can help you anticipate what is coming and feel more in control.
This journey is commonly broken down into four distinct phases. It is important to remember that not everyone experiences all four stages, and their timing and intensity can vary significantly from person to person and even from one attack to the next.
The infographic below illustrates how a migraine attack can progress, often beginning with changes in the brain long before the pain starts.
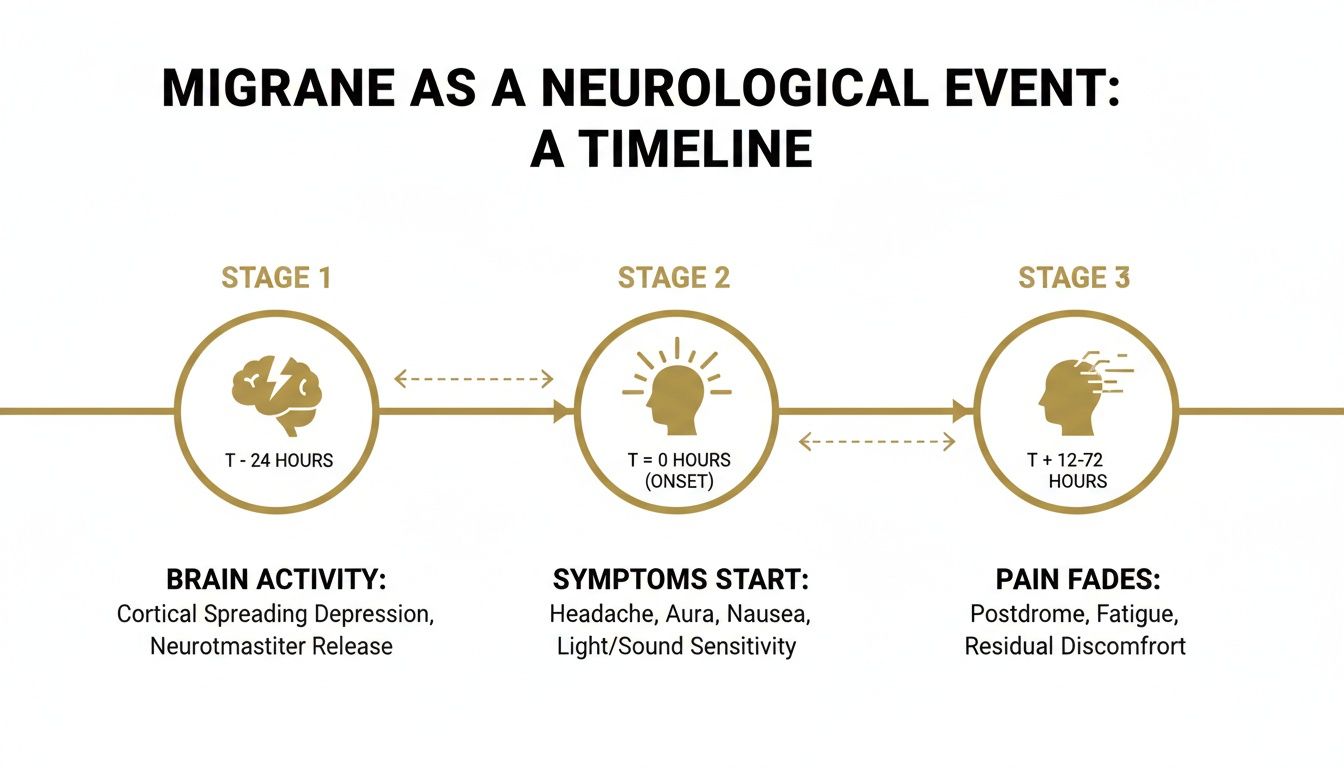
This visual timeline helps show that the headache itself is just one piece of a much larger puzzle.
To help clarify what a full migraine attack can involve, the four phases are broken down below. The table provides a quick overview of each stage, from the first subtle warnings to the final recovery period.
Understanding the Four Phases of a Migraine
| Phase | Typical Onset | Common Symptoms | Key Characteristics |
|---|---|---|---|
| Prodrome | 24-48 hours before the headache | Mood swings, neck stiffness, food cravings, yawning, fatigue | Subtle "warning signs" that the brain is preparing for an attack. |
| Aura | 5-60 minutes before or during the headache | Visual disturbances (flashing lights, blind spots), tingling sensations, speech difficulty | Temporary neurological symptoms that are completely reversible. Affects about 25-30% of people. |
| Headache | Can last 4-72 hours | Throbbing pain (often one-sided), nausea, vomiting, extreme sensitivity to light and sound | The most intense and disabling phase, often forcing the person to rest. |
| Postdrome | 24-48 hours after the headache | Exhaustion, mental fogginess ("migraine hangover"), difficulty concentrating, scalp sensitivity | The recovery period where the brain and body slowly return to normal. |
Each phase has its own distinct characteristics. Understanding them is a key step toward managing your migraines more effectively.
Phase 1: The Prodrome (Pre-Headache)
The prodrome can be thought of as an early warning system. These are subtle shifts that may begin a few hours to a day or more before the headache phase. Up to 77% of people with migraine report noticing these premonitory symptoms.
The signs can be vague and easy to dismiss. Learning to spot them involves becoming familiar with your personal migraine patterns.
Common prodrome symptoms include:
- Mood Changes: Suddenly feeling irritable, low, or even unusually energetic for no apparent reason.
- Neck Stiffness: A distinct ache or tightness in the neck is a very common early sign.
- Food Cravings: An intense, specific craving for certain foods, often sweet or salty.
- Increased Yawning: You might find yourself yawning much more than usual without feeling tired.
- Fatigue: A deep sense of exhaustion that doesn't seem to match your recent activity level.
These early symptoms are thought to originate from changes in the hypothalamus, a part of the brain that acts as the body's primary regulator.
Phase 2: The Aura
Experienced by about 25% to 30% of people with migraine, the aura consists of temporary neurological symptoms that usually appear just before or during the headache. An aura tends to develop gradually over about five minutes and can last up to an hour.
Visual disturbances are the most common type of aura, but other senses can also be affected.
An aura is understood to be the direct result of cortical spreading depression, that slow wave of electrical activity moving across the brain's surface. The specific symptoms depend entirely on which part of the brain this wave is passing through.
Classic examples of aura include:
- Visual Disturbances: Seeing flashing lights, blind spots, shimmering zig-zag lines, or geometric shapes.
- Sensory Changes: A pins-and-needles or numb sensation that often starts in the fingers and moves up the arm to the face.
- Speech Difficulties: Trouble finding the right words or speaking clearly (a condition known as transient aphasia).
While an aura can be a disorienting experience, it is temporary and fully reversible.
Phase 3: The Headache (Attack)
This is the phase most people associate with migraine, and it is often the most debilitating. The headache is typically moderate to severe and can last anywhere from four to 72 hours if untreated.
The pain is often described as a throbbing or pulsing sensation, usually on one side of the head, although it can affect both. Routine physical activity, like climbing stairs, can make the pain worse.
This phase also brings a cluster of other significant symptoms:
- Nausea and Vomiting: A large number of people experience intense nausea during an attack.
- Photophobia: Extreme sensitivity to light, often creating an overwhelming need for a dark room.
- Phonophobia: Extreme sensitivity to sound, where normal noises can feel unbearably loud.
During the headache phase, the brain is in a state of high alert, with its pain pathways fully activated.
Phase 4: The Postdrome (Migraine Hangover)
The end of the headache pain does not always mean the migraine is over. Many people then enter the postdrome phase, often called the "migraine hangover," which can last for another 24 to 48 hours.
In this final stage, you might feel completely drained, similar to recovering from an illness. It can be difficult to concentrate, and your thinking may feel foggy or slow. Some people also report scalp tenderness.
This phase is a powerful reminder that a migraine is a major neurological event. It takes time for the brain and body to recover and return to their normal state.
How to Differentiate Migraine From Other Headaches
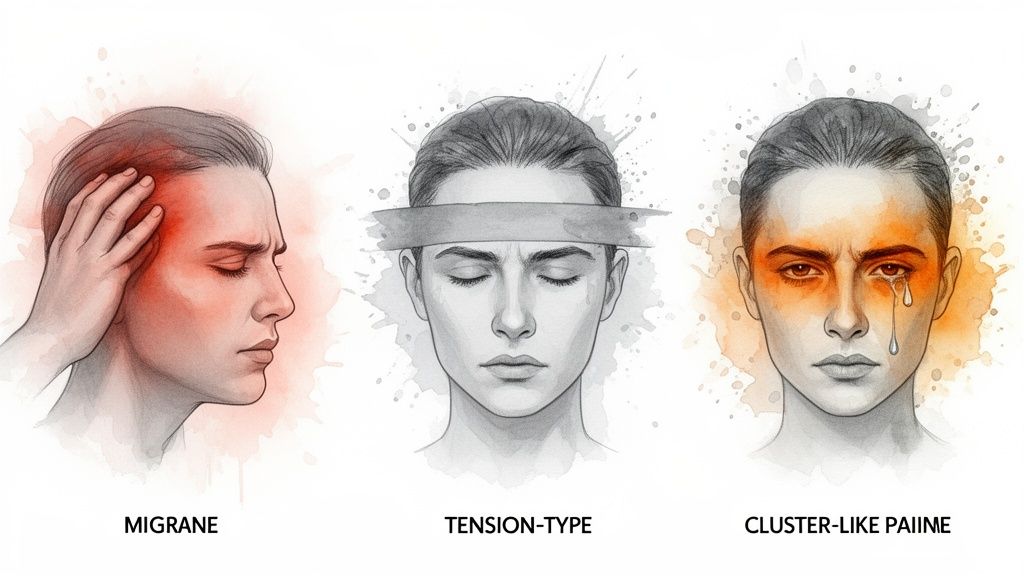
Telling a migraine apart from other types of headaches is a critical step toward getting the right support. Clinicians look for specific patterns and a combination of symptoms to make an accurate diagnosis.
Understanding these different profiles helps you describe your experience more clearly to a healthcare professional. This clarity is essential for receiving a correct diagnosis and an effective treatment plan.
Understanding Tension-Type Headaches
When people refer to a "normal" headache, they are usually describing a tension-type headache. This is the most common type, typically causing a dull, persistent ache or a sensation of pressure, often likened to a tight band around the head.
The key difference is that tension headaches usually affect both sides of the head and are not typically severe enough to prevent daily activities. They rarely come with the nausea or extreme sensitivity to light and sound that are hallmarks of a migraine. For those who experience this type of pain, exploring natural remedies for tension headaches may be a useful starting point.
The Intensity of Cluster Headaches
Cluster headaches are much less common but are known for being exceptionally painful. They are considered one of the most severe pain conditions. The pain is often described as a sharp, burning, or piercing sensation.
Their most defining feature is their location: almost always one-sided and centered around one eye. These attacks occur in cyclical patterns, or "clusters," which can last for weeks or months. During an attack, associated symptoms may include a blocked or runny nose, a drooping eyelid, or facial sweating, all on the same side as the pain. The sheer severity and these distinct autonomic symptoms clearly set cluster headaches apart from migraines.
Recognising the Migraine Profile
So, what makes a migraine distinct? It's not just the pain; it’s the full package of symptoms that create a recognisable pattern.
The real clue is often the company the headache keeps. A severe headache on its own might not be a migraine. But when that same headache is accompanied by nausea and sensory disturbances, the clinical picture starts to look much more like a migraine.
Healthcare professionals look for these classic migraine headache symptoms:
- Pain Quality: The pain is usually moderate to severe with a distinct throbbing or pulsing quality.
- Location: It typically affects just one side of the head, though it can switch sides or occasionally be on both.
- Associated Symptoms: Nausea is very common and can be severe enough to cause vomiting.
- Sensory Sensitivity: Heightened sensitivity to light (photophobia) and sound (phonophobia) is a major feature.
It's also worth noting that some conditions, such as TMJ disorders, can cause headaches with symptoms that overlap with migraines. For some, investigating TMJ and headache migraine therapy may be an important part of finding relief.
To make the differences clearer, here is a side-by-side comparison.
Migraine vs. Tension vs. Cluster Headaches
| Feature | Migraine Headache | Tension-Type Headache | Cluster Headache |
|---|---|---|---|
| Pain Location | Usually one side of the head | Both sides, often in a band-like pattern | Behind or around one eye, strictly one-sided |
| Pain Quality | Throbbing, pulsing | Dull, aching, or a feeling of pressure | Severe, sharp, stabbing, or burning |
| Pain Intensity | Moderate to severe | Mild to moderate | Excruciating, often described as one of the worst pains imaginable |
| Duration | 4 to 72 hours | 30 minutes to 7 days | 15 minutes to 3 hours, occurring in clusters over weeks or months |
| Associated Symptoms | Nausea, vomiting, extreme sensitivity to light and sound, aura in about 25% of cases | None, or mild sensitivity to light or sound, but not both | Drooping eyelid, runny or blocked nose, facial sweating, restlessness, and agitation |
This table illustrates how different these conditions are, which is why a proper diagnosis is so important for effective management.
When to Seek Medical Advice for Your Headaches

Most headaches, including severe migraines, are not a sign of a more serious underlying issue. However, it is crucial to know when a headache might indicate something else. Certain symptoms are considered 'red flags'—warning signs that healthcare professionals are trained to take very seriously.
Knowing what to look for is not about causing anxiety; it is about safety. It helps you know when to manage a typical attack and when to act quickly if something feels different.
Urgent Red Flag Symptoms
Some headache symptoms require immediate medical attention to rule out more serious conditions. If you experience any of the following, you should seek urgent care.
- A sudden, severe headache that reaches its peak within a minute, often described as the ‘worst headache of your life’. This is sometimes called a thunderclap headache.
- A headache accompanied by a fever, stiff neck, confusion, a seizure, or double vision.
- Weakness, numbness, or paralysis on one side of your body.
- Difficulty speaking or understanding others.
You should also be evaluated if you develop a headache after a head injury, or if you have a headache that gets progressively worse over several days.
When to See Your GP for Ongoing Migraines
Even without red flag symptoms, living with frequent or severe headaches is a valid reason to see your doctor. Getting a proper diagnosis from your GP is the essential first step towards finding a treatment plan that works for you.
It may be time to book an appointment if:
- Your migraine attacks are becoming more frequent or more intense.
- Over-the-counter pain relief is no longer effective.
- The attacks are significantly disrupting your work, family life, or social activities.
- You want to explore preventive treatments, such as whether Botox for migraines could be an appropriate option.
Your GP can help you develop a management plan that goes beyond simply reacting to attacks. It is worth noting that accessing specialist care can sometimes be challenging. In the UK, waiting times for headache clinics have increased, with some reports in 2023 suggesting waits of over six months. This, combined with a shortage of trained specialists, can cause delays.
These challenges make that initial conversation with your GP an even more vital first step.
A Clearer Path to Managing Your Migraines
Effectively managing migraines begins with understanding the patterns behind the attacks. This article has aimed to provide a clearer picture of what a migraine is: a complex neurological event that unfolds in phases, not just an isolated, severe headache.
You should now be better able to identify the key symptoms and, crucially, understand how they differentiate a migraine from other types of headaches. This knowledge is a valuable tool. It helps you become a more careful observer of your own body, which in turn allows for more productive conversations with your doctor.
From Knowledge to Action
Moving from confusion to clarity can be transformative. It allows you to ask more informed questions and make considered decisions about your health, from lifestyle adjustments to treatment options. For example, distinguishing between your triggers and the early prodrome symptoms can change how you approach your daily routine.
For those interested in exploring proactive strategies, our article on supplements for migraines examines another aspect of migraine care.
While articles like this one can clarify the problem, they often cannot provide the organised, step-by-step framework needed for long-term management. Blogs are useful for explaining specific concepts, but true confidence comes from understanding how all the pieces fit together.
Gaining control over migraines is rarely about a single solution. It is about consistently applying a structured understanding of your unique patterns and triggers over time.
For readers wanting a structured overview to build a comprehensive plan, we created The Migraine Guide. It is designed to bring these concepts into a single, cohesive resource, providing a roadmap to navigate your health with more confidence.
Common Questions About Migraine
Let's conclude by addressing some frequently asked questions about migraine. Clear, straightforward answers can help reduce uncertainty.
Can You Have a Migraine Without the Headache?
Yes, it is possible. This is sometimes referred to as an 'acephalgic migraine' or 'silent migraine'.
This means you might experience all the typical symptoms of the aura phase—such as flashing lights, zig-zag lines, or pins and needles—but the headache pain itself never develops. You could still feel nauseous, dizzy, or sensitive to light and sound. It is still considered a migraine because the same underlying neurological event is occurring in the brain; it just doesn't manifest with the pain phase.
What Usually Triggers a Migraine?
This can be complex because triggers are highly individual. What sets off a migraine in one person may have no effect on another. However, through clinical experience, some common patterns emerge.
Commonly reported triggers include:
- Stress: Both acute stress and the let-down period after stress can be triggers.
- Sleep Disruption: Too little sleep, too much sleep, or inconsistent sleep patterns are often cited.
- Hormonal Changes: Many women find their migraines are linked to their menstrual cycle.
- Environmental Factors: Bright or flickering lights, strong smells, or changes in weather can be triggers for some.
- Food and Drink: Certain items are frequently mentioned, including aged cheeses, red wine, and processed meats containing nitrates.
The most effective way to identify your personal triggers is often through careful observation. Keeping a simple diary of your symptoms and noting what you were doing, eating, or feeling beforehand can be very revealing.
How Long Does a Migraine Attack Actually Last?
The main headache phase typically lasts anywhere from 4 to 72 hours if left untreated.
However, the entire migraine experience is often longer. You might feel 'off' for a day or two before the pain starts (the prodrome), and then feel drained and foggy for another day or two after it has gone (the postdrome). This "migraine hangover" is a very real part of the attack for many people.
At The Patients Guide, we believe that structured knowledge is the key to managing your health with confidence. While this article provides clarity, our guides offer the step-by-step framework needed for long-term understanding.
For a comprehensive resource designed to connect all these concepts, explore our full library of health guides at https://www.thepatientsguide.co.uk.
Also in Migraines

Finding Clear Help with Migraines: A Grounded Guide
February 25, 2026 13 min read
Feeling overwhelmed? Get clear, evidence-based help with migraines. This guide explains how to manage symptoms, track triggers, and talk to your doctor.
Read More

Understanding Ocular Migraine Symptoms and Triggers
February 19, 2026 14 min read
A clear, reassuring guide to understanding ocular migraine. Learn to identify symptoms, understand triggers, and know when to seek professional care.
Read More

Understanding Migraine Vestibular Vertigo
February 17, 2026 12 min read
A clear guide to understanding migraine vestibular vertigo. Learn to recognize its symptoms, understand the causes, and explore effective management strategies.
Read More
Subscribe
Sign up to get the latest on updates, new releases and more …
