Modern healthcare is fragmented. Understanding your condition helps connect the dots.
Modern healthcare is fragmented. Understanding your condition helps connect the dots.
Library
FEATURED
HEALTH HIGHLIGHT
FEATURED

Understand your triggers, find relief that works, and stop migraines from ruling your life.
HEALTH HIGHLIGHT

Learn how to protect your bones, reduce risk of fractures, and take charge of your bone health at any age.
MINI GUIDES

Get quick answers, learn proven tips, and take action with our bite-size mini guides.
Botox for Migraines: A UK Guide to Treatment and Expectations
January 29, 2026 11 min read

If you are exploring Botox for chronic migraines, it is likely you have already navigated a long and often frustrating journey. You may have tried several other treatments with limited success, and the information online can feel like a confusing mix of cosmetic claims and dense clinical data. It can be difficult to determine if this is a genuinely viable option for you.
This guide is designed to provide a clear, grounded explanation of how Botox is used as a medical treatment for chronic migraine. Our goal is to move past the hype and offer the kind of information that supports a confident and informed conversation with your doctor.
Understanding Botox as a Migraine Treatment

Living with chronic migraine can be isolating. When standard medications and lifestyle adjustments do not provide enough relief, it is reasonable to consider other established options. One of these is Botox (onabotulinumtoxinA), an approved preventative treatment in the UK.
Most people associate Botox with cosmetic procedures, which is an understandable point of confusion. Its role in migraine management, however, is purely medical and operates on a completely different principle. The aim is not to smooth wrinkles but to interrupt the pain signals that drive a migraine attack.
Setting Realistic Expectations
It is important to approach this treatment with a balanced perspective. For many individuals, Botox can significantly reduce the number of headache days they experience each month. However, it is not a cure, and its effectiveness can vary from person to person.
In a clinical setting, this treatment is typically considered if you meet specific criteria:
- A Chronic Migraine Diagnosis: This generally means you experience headaches on 15 or more days per month, with at least eight of those days having migraine features.
- Previous Treatment Attempts: In the UK, you will usually need to have tried at least three other preventative medications that were either ineffective or not well-tolerated.
The crucial distinction is that Botox for migraines is a preventative therapy. The objective is to reduce the frequency and severity of attacks over time, not to stop a migraine that is already in progress. This helps clarify its place in a long-term management plan.
This is not about a miracle cure. It is about exploring a well-established, evidence-backed option for managing a complex condition. For more general information, you can learn about various migraine management strategies in our other articles.
How Does Botox Work for Migraines?
When most people think of Botox, they picture its effect on muscles. For treating chronic migraine, however, its function is more complex. It is about interrupting the signals that trigger a migraine before an attack can fully develop.
While Botox does relax muscles, its primary mechanism in migraine prevention relates to its effect on nerve endings. In individuals with chronic migraine, the nerves around the head and neck can exist in a state of high alert, becoming hypersensitive to stimuli.
These nerves are primed to release a cascade of chemicals that signal pain to the brain. A key chemical in this process is CGRP (calcitonin gene-related peptide), which is known to play a significant role in escalating migraine pain.
Interrupting the Nerve-to-Brain Signal
This is where Botox intervenes. When injected into specific points around the head and neck, it is absorbed by these overactive nerve endings. Once inside, it functions as a roadblock, physically preventing the nerves from releasing their pain-transmitting chemicals.
By blocking the release of CGRP and other pain messengers, Botox can stop or reduce the intensity of pain signals reaching the brain. This interruption can help break the cycle of pain before it begins.
The mechanism is not primarily about the muscle relaxation seen in cosmetic use; it is a chemical block at the nerve level. This is why the injections follow a precise protocol—to target the key nerve pathways involved in transmitting migraine signals.
A Proactive, Not Reactive, Approach
This explains why Botox is a purely preventative treatment. It is not an acute medication used once a migraine has started, as it requires time to be absorbed by nerve endings and begin blocking signals. The effect is cumulative, building over time with regular treatments.
Many people find the benefits become more apparent after their second or third round of injections, which are typically scheduled 12 weeks apart. This gradual improvement occurs because with each treatment, more of those over-sensitised nerve pathways are quieted, making it more difficult for usual triggers to initiate an attack.
For readers wanting a structured overview of how preventative treatments fit into a comprehensive management plan, this is explored in more detail in our Migraine Guide.
What to Expect During a Botox Treatment Session
It is normal to feel some apprehension before a new medical procedure. The process for receiving Botox for migraines is a straightforward and well-established protocol in the UK. Understanding the steps can help reduce uncertainty.
The appointment itself is relatively brief, often completed in about 15 minutes. Your clinician will ensure you are comfortable, answer any final questions, and then begin the procedure. Most people describe the injections as small, brief pinpricks.
The Injection Process Explained
The treatment follows a specific, evidence-based protocol known as PREEMPT. This is not an arbitrary approach; it is a targeted procedure involving 31 small injections into shallow muscles around the head and neck, using a very fine needle.
These injection sites are mapped across seven key muscle areas known to be involved in migraine pathways:
- Forehead
- Between the eyebrows (glabella)
- Temples
- Back of the head (occipitalis)
- Upper neck (cervical paraspinal)
- Upper back and shoulders (trapezius)
Each injection is intended to calm the overactive nerve endings in these zones, helping to inhibit migraine pain signals. The procedure is performed in a way that should not impact your natural facial expressions.
Visualising the Path to Prevention
This diagram illustrates how Botox can act as a roadblock for pain signals, preventing them from reaching the brain and initiating a migraine.
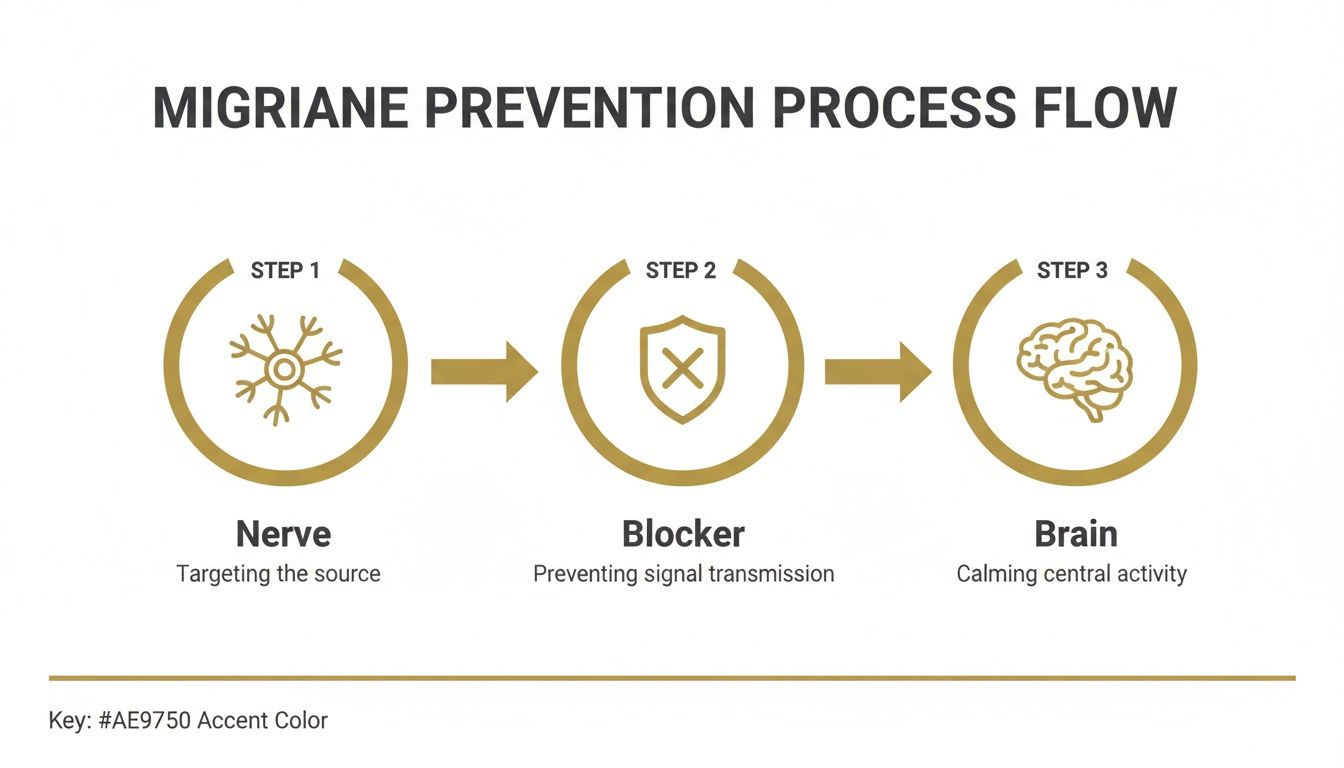
It functions as an intermediary, stepping in between sensitised nerves and the brain’s pain centres to help break the cycle.
After the Procedure
There is typically no downtime required after the treatment. You can usually return to your daily activities immediately, whether that is driving home or going back to work.
Your clinician may provide simple aftercare instructions, such as avoiding rubbing the injection sites or postponing strenuous exercise for the remainder of the day. This is a precaution to ensure the Botox remains localised to the treatment areas.
It is important to remember that the results are not immediate. The preventative effects build gradually, which is why treatments are scheduled every 12 weeks. Tracking your migraine frequency and severity is very helpful for assessing its effectiveness. Using a simple tool, like our Migraine Diary Template, can make it easier to monitor your progress between appointments.
How Effective Is Botox for Chronic Migraines?
For anyone considering a new treatment for chronic migraine, the primary question is straightforward: how well does it work? For Botox, the evidence is reassuring, supported by years of clinical research and real-world application. It is also important to maintain realistic expectations.
Success is generally not measured as a complete cure but as a significant reduction in headache frequency and severity. The goal is to reclaim headache-free days and improve overall quality of life.
What the Research Shows
The use of Botox for migraines is based on evidence from two major clinical trials known as the PREEMPT studies. These were large-scale, placebo-controlled trials that provided clear data on its efficacy.
The findings were consistent and clinically meaningful. On average, patients treated with Botox experienced eight to nine fewer headache days per month compared to their baseline. For someone living with near-daily head pain, such a reduction can be transformative.
In clinical practice, treatment is often considered successful if a patient experiences at least a 50% reduction in their monthly migraine days. This provides a clear, measurable benchmark for a significant improvement in daily functioning.
Benefits Often Build Over Time
It is important to understand that the effects of Botox are often cumulative. This means the relief experienced after the third or fourth treatment cycle may be greater than what was felt after the first.
Patience is therefore a key component of the process. Your doctor will likely recommend committing to at least two treatment cycles (approximately six months) before making a final assessment of its suitability for you.
Typical Improvement Rates with Botox Treatment
Data from clinical practice shows a clear trend: the longer patients continue with the treatment, the more likely they are to experience significant benefits.
| Timepoint | Patients with ≥50% Fewer Migraine Days |
|---|---|
| After 2 treatments (24 weeks) | ~47% |
| After 5 treatments (60 weeks) | ~70% |
As shown in studies published by PMC NCBI, nearly half of patients achieve the 50% reduction benchmark by the second treatment. By the fifth treatment, this figure rises to approximately 70%. This data highlights the importance of allowing the treatment sufficient time to work.
Does It Work for Everyone?
It is also true that Botox does not work for every individual. A minority of people may not respond to the treatment, or may find the side effects outweigh the benefits. This is a reality for all preventative migraine therapies.
The reasons for this variability are not always fully understood but likely involve individual differences in nerve pathways and pain processing. This is why a close partnership with your doctor is so important for tracking progress and determining the best path forward.
For a more detailed look at the clinical evidence, our Migraine Patient's Guide References page offers further resources.
Understanding Potential Risks and Side Effects
When considering any medical treatment, it is essential to have a balanced understanding of potential side effects alongside the benefits. With Botox for migraines, most side effects are mild, temporary, and localised to the injection areas.
Clinicians experienced in this procedure are familiar with these potential effects, which are generally predictable and manageable. The purpose of this information is not to cause alarm, but to provide transparency so you can have an informed discussion with your doctor.
Common and Localised Side Effects
The most frequently reported side effects are directly related to the injections. A mild, local reaction is a common response to the procedure.
These may include:
- Neck pain or stiffness: This is one of the most common effects. It typically feels like muscle soreness and tends to resolve within a few days to a couple of weeks.
- Muscle weakness or tightness: A temporary feeling of weakness may occur in the muscles around the injection sites, particularly in the neck and shoulders.
- Headache: Ironically, some individuals experience a mild headache shortly after treatment. This is usually transient and less severe than a migraine.
- Bruising or swelling: Minor bruising or puffiness at the injection sites is possible and typically fades within a few days.
These are generally considered temporary reactions to the procedure itself.
Less Common Side Effects
Beyond these common reactions, a few other side effects may occur, though they are less frequent. These can happen if the Botox spreads slightly from the intended muscle to an adjacent one.
A side effect people often ask about is a drooping eyelid, known clinically as ptosis. While it sounds concerning, it is uncommon. It occurs if the toxin migrates into the small muscle that elevates the eyelid and typically resolves on its own as the Botox wears off.
Other less common effects might include flu-like symptoms, blurred vision, or dry eyes. These are almost always mild and temporary. Serious side effects are extremely rare, and your clinician will discuss all potential risks with you beforehand.
The skill of the practitioner is a significant factor here. An expert trained in the specific PREEMPT protocol for chronic migraine understands the precise anatomy to target, which can increase effectiveness and reduce the risk of side effects.
Accessing Botox for Migraines in the UK
Navigating the healthcare system to access a specialist treatment like Botox can seem complex. In the UK, there are two main pathways: through the NHS or via private healthcare. Understanding the requirements for each can help you prepare for conversations with your doctor.
Your GP is typically the first point of contact. They can review your migraine history and, if appropriate, refer you to a neurologist or a specialist headache clinic. A formal diagnosis of chronic migraine is required before Botox can be considered through either route.
NHS Eligibility and NICE Guidelines
Access to this treatment on the NHS is governed by guidelines from the National Institute for Health and Care Excellence (NICE). These guidelines ensure Botox is offered to patients who are most likely to benefit, particularly when other treatments have been unsuccessful.
To be considered for Botox for migraines on the NHS, you generally need to meet the following criteria:
- You have a diagnosis of chronic migraine, defined as headaches on 15 or more days a month, with at least eight of those being migraine days.
- You have tried at least three different oral preventative medications without success, either due to lack of efficacy or intolerable side effects.
If you meet these criteria, your GP can refer you to a specialist who will confirm your eligibility and can administer the treatment. It is worth noting that there may be a waiting list for specialist appointments.
Private Treatment Options
If you do not meet the NICE criteria or prefer to avoid NHS waiting times, seeking treatment privately is an alternative. You can book directly with a private neurologist or a clinic specialising in headache and migraine treatment.
The primary difference is the cost. In the private sector, you are responsible for the consultation fees and the full price of the treatment.
In the UK, a single private session of Botox for migraines typically costs between £500 and £750. This fee usually covers the specialist's consultation, the Botox medication itself, and the procedure. As treatments are repeated every 12 weeks, this represents a significant ongoing financial commitment.
The Evidence That Led to UK Approval
The approval of Botox for chronic migraine in the UK was based on robust scientific evidence. The pivotal PREEMPT trials (Phase III Research Evaluating Migraine Prophylaxis Therapy) demonstrated that patients receiving the treatment experienced a significant reduction in headache frequency.
The results showed an average reduction of eight to nine headache days per month after two treatment cycles. This strong evidence led NICE to approve its use for chronic migraine in 2012, establishing it as an important treatment option in the UK. You can read more about the trials behind Botox for migraines on the Harley Street Skin Clinic's website.
Common Questions About Botox for Migraines
Even with a clear understanding of the process, it is natural to have additional questions. Here are answers to some of the most common queries people have when considering this treatment.
How Long Does It Take for Botox to Start Working?
While some individuals may notice a difference sooner, it is best to be patient. Most specialists advise that it can take two full treatment cycles—approximately 24 weeks—to experience the full benefits.
The effects tend to be cumulative, meaning the improvement seen after the second round of injections is often greater than after the first. It is therefore important to complete at least two sessions before you and your doctor fully assess its effectiveness for you.
Is the Botox Injection Procedure Painful?
Most people report that the injections are more of a mild discomfort than truly painful. The needles used are extremely fine, similar to those used in acupuncture, and the injections are shallow.
The sensation is often described as a brief, small pinch at each of the 31 injection sites. As the entire procedure is typically completed in about 15 minutes, any discomfort is short-lived.
Many patients feel that the brief sensation from the injections is minor compared to the debilitating pain of a migraine attack.
Will Botox for Migraines Affect My Facial Expressions?
This is a reasonable concern given Botox's cosmetic applications. However, the injection protocol for migraines is entirely different. The goal is to target specific nerve endings involved in pain signalling, not the primary muscles used for facial expressions.
The injection sites are mostly separate from the muscles that control expressions like smiling or frowning. While a minor change, such as a slight brow lift, is a possible side effect, it is not common. A practitioner properly trained in the PREEMPT protocol for migraine should not cause significant changes to your facial movement.
What Happens If I Decide to Stop the Treatments?
If you choose to discontinue Botox, the process is simple. The effects of the botulinum toxin will gradually wear off over the following months, and your migraine patterns will likely return to what they were before treatment.
There are no permanent changes to your muscles or nerves from the treatment, and there are no withdrawal symptoms. This allows you and your doctor to regularly review whether continuing with the therapy remains the best approach for managing your migraines.
At The Patients Guide, we believe clear, structured information is the first step towards feeling more in control of your health. While articles provide valuable insight, they are just one piece of the puzzle. For those who want to go beyond individual topics and see the bigger picture, a more organised resource can make all the difference.
Our guides are created to connect the dots between symptoms, treatments, and lifestyle choices, offering a comprehensive roadmap for conditions like migraine. They are designed to support your conversations with healthcare professionals and empower your daily decisions.
If you are looking for a step-by-step framework to manage your health with confidence, explore our full library of guides.
Also in Migraines

Finding Clear Help with Migraines: A Grounded Guide
February 25, 2026 13 min read
Feeling overwhelmed? Get clear, evidence-based help with migraines. This guide explains how to manage symptoms, track triggers, and talk to your doctor.
Read More

Understanding Ocular Migraine Symptoms and Triggers
February 19, 2026 14 min read
A clear, reassuring guide to understanding ocular migraine. Learn to identify symptoms, understand triggers, and know when to seek professional care.
Read More

Understanding Migraine Vestibular Vertigo
February 17, 2026 12 min read
A clear guide to understanding migraine vestibular vertigo. Learn to recognize its symptoms, understand the causes, and explore effective management strategies.
Read More
Subscribe
Sign up to get the latest on updates, new releases and more …
